Lower Back Pain: Common Triggers and Fast Relief Steps
Lower back pain can come on suddenly after lifting a suitcase, or creep up after weeks of long commutes and desk work. Either way, it can be alarming and very d...
Jan 30, 2026

Lower back pain can come on suddenly after lifting a suitcase, or creep up after weeks of long commutes and desk work. Either way, it can be alarming and very disruptive.
The good news is that most episodes are not caused by anything serious and often improve with the right self-care and early, sensible movement.
This guide breaks down common lower back pain triggers and fast relief steps you can start today, plus clear signs that you should seek urgent medical help.
What “lower back pain” actually means
“Lower back pain” usually refers to pain between the bottom of your ribs and the top of your pelvis (the lumbar spine area).
It may feel local and stiff (often worse after sitting), or like it spreads into the buttock or thigh.
If pain runs down the leg with tingling, numbness, or weakness, that may involve nerve irritation (often described as sciatica) and deserves closer assessment.
Clinicians often describe low back pain by duration:
Acute: up to 6 weeks
Subacute: 6 to 12 weeks
Persistent/chronic: more than 12 weeks
According to the UK NHS guidance on back pain, most back pain improves within a few weeks.
Common triggers of lower back pain (and why they hurt)
Lower back pain is often “non-specific”, meaning it is not tied to one identifiable structure on a scan.
That does not mean it is “all in your head”. It often reflects a mix of temporary tissue irritation, muscle guarding, and sensitivity in the nervous system during a flare.
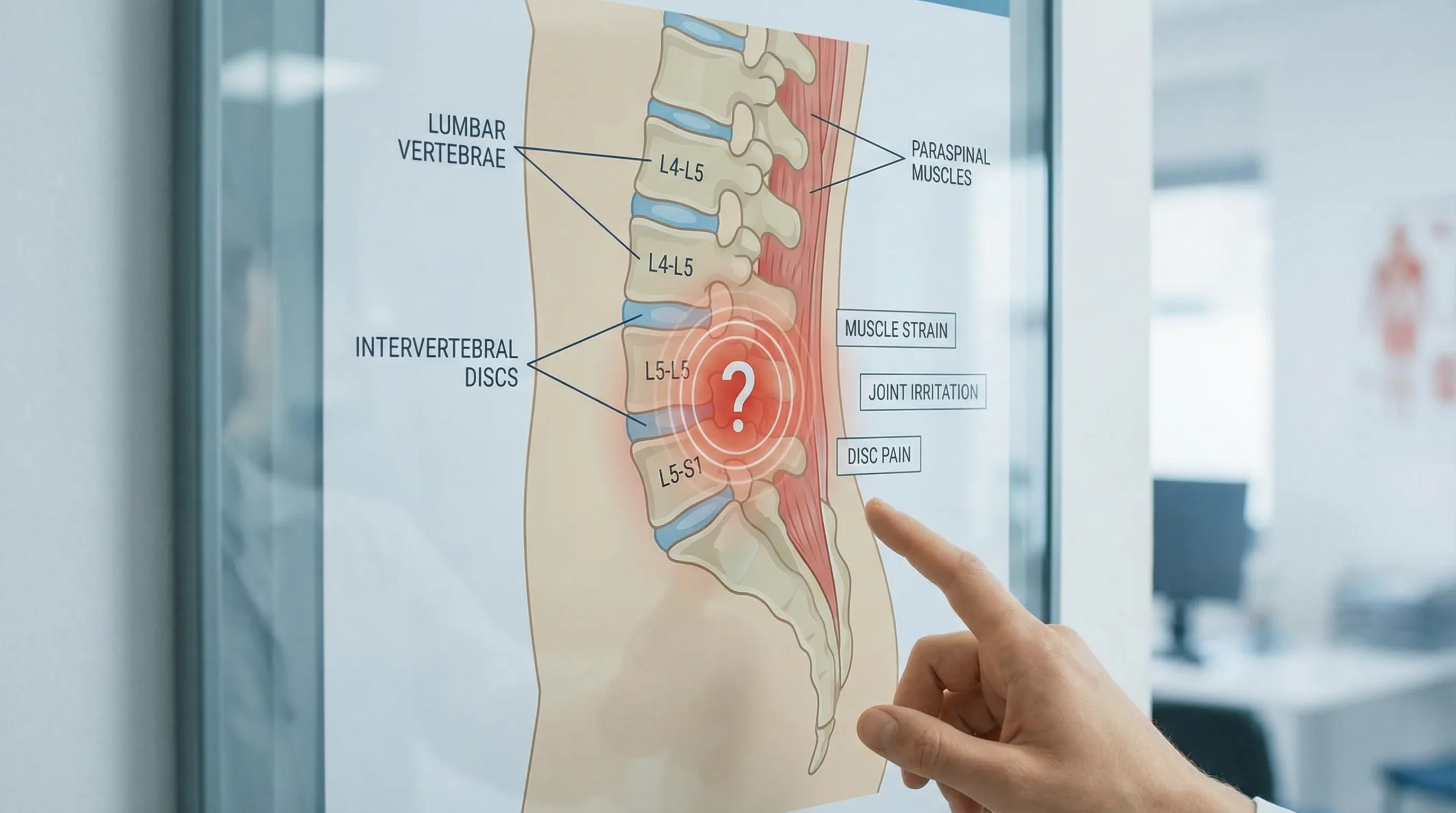
The most common triggers
Sudden overload (lifting, twisting, awkward carries): unprepared tissues get irritated, muscles may tighten to protect the area.
Prolonged sitting (especially without breaks): sustained positions can increase stiffness and load the same structures repeatedly.
Rapid spike in activity (the weekend warrior effect): demand exceeds your current capacity.
Poor sleep and high stress: can increase pain sensitivity and promote bracing (constant muscle tension).
Hip stiffness and reduced glute/core capacity: the low back takes more load during everyday movement.
Disc-related irritation (sometimes with leg symptoms): imaging alone does not explain symptoms, assessment is more useful.
Joint irritation (facet joints or sacroiliac joint): often one-sided stiffness, worse with certain movements.
Pregnancy and post-partum changes: changing loads through the pelvis and new demands can trigger pain.
Quick reference: trigger to first-step response
Common trigger | Typical pattern | First step you can try today |
|---|---|---|
Lifting/twisting strain | Sharp catch, sore muscles, worse with bending | Gentle walking + heat + avoid heavy lifting for 24 to 48 hours |
Prolonged sitting | Stiffness on standing, dull ache | Stand up every 30 to 45 minutes, do 60 seconds of easy mobility |
Rapid spike in exercise | Soreness plus movement pain after activity | Reduce load, keep moving, return gradually over 1 to 2 weeks |
Stress/poor sleep | Diffuse tightness, flare ups with busy periods | Breathing + short walks + prioritise sleep comfort |
Possible nerve irritation | Pain into buttock/leg, tingling | Avoid forcing stretches, seek assessment if symptoms persist or worsen |
Fast relief steps for lower back pain (first 24 to 72 hours)
The goal early on is to calm symptoms, keep you safely moving, and reduce the risk of a short-term flare turning into a longer problem.
1) Keep moving, but reduce the dose
UK guidance generally supports staying active within tolerance for non-specific low back pain.
The NHS advises continuing normal activities as much as possible rather than prolonged bed rest.
Practical options:
Short walks (5 to 10 minutes) spaced through the day
Gentle movement breaks after sitting
Temporarily avoiding movements that reliably spike pain sharply
A helpful rule of thumb is to scale activity to symptoms.
If you feel looser afterwards, that is usually a good sign.
If pain escalates and stays elevated for hours, do less next time.
2) Find positions of comfort
Small position changes often help quickly.
Side lying: pillow between knees
On your back: pillow under knees
Sitting: hips slightly higher than knees (cushion), feet flat, gentle support at the lower back
You are not chasing “perfect posture”.
You are looking for a position that reduces symptoms and lets you relax.
3) Use heat (or cold)
Many people find heat helpful for stiffness and muscle spasm (hot shower, heat pack).
Some prefer cold in the first 24 hours after a sudden strain.
Use whichever reduces your pain.
Practical tip: 15 to 20 minutes, with a barrier (towel) between skin and heat/cold source.
4) Consider over-the-counter pain relief safely
Pain relief can help you keep moving, which often supports recovery.
In the UK, NICE guidance on low back pain and sciatica (NG59) discusses medication options and cautions.
Because the safest option depends on your medical history and other medications, speak to a pharmacist or GP if you are unsure.
Avoid combining medications without professional advice.
5) Try a 5-minute gentle “reset”
Aim for easy motion rather than deep stretching.
Choose 2 to 3 options and keep discomfort mild:
Easy walking: 2 minutes
Pelvic tilts (lying on back, knees bent): 60 seconds
Knee rolls (lying on back, knees bent, gently side to side): 60 seconds
Cat-camel (hands and knees): 6 to 10 slow reps
If you have leg tingling or numbness, avoid forcing stretches that reproduce nerve pain.
6) Make one ergonomic change today
You do not need a full office overhaul to get relief.

Try one:
Set a timer to stand up every 30 to 45 minutes
Place a small cushion or rolled towel at your lower back
Bring your screen up so you are not leaning forward for long periods
When lower back pain needs urgent medical attention (red flags)
Most back pain is not serious, but certain symptoms should be checked urgently.
Red flag symptom | Why it matters | What to do |
|---|---|---|
New trouble controlling bladder or bowel, or numbness in the saddle area | Possible cauda equina syndrome | Seek emergency medical care immediately |
Severe or progressive weakness in the leg/foot | Possible significant nerve compromise | Urgent medical assessment |
Back pain with fever, feeling very unwell, or unexplained weight loss | Possible infection or systemic illness | Same-day GP/urgent care |
Significant trauma (fall, accident), or osteoporosis risk | Possible fracture | Urgent assessment |
History of cancer with new, persistent back pain | Needs medical evaluation | Urgent GP appointment |
Constant, worsening pain that does not change with position, especially night pain | Needs medical evaluation | GP/urgent care |
If you are unsure, contact NHS 111 or your GP for guidance.
How osteopathy can help lower back pain (beyond quick fixes)
Fast relief matters, but so does preventing the next flare.
An osteopathic approach commonly combines symptom relief with addressing contributing factors like movement patterns, joint and soft tissue irritation, and load management.
This often includes assessment, manual therapy where appropriate, advice on pacing and return to work or sport, and a simple home plan.
If your symptoms make travel difficult or you want guidance quickly, virtual consultations can be useful for triage, education, and building a safe movement plan.
You can learn more about care options at Versano Clinics.
Preventing lower back pain from coming back
Recurrence is common, but it is not inevitable.
Prevention usually comes down to gradually building capacity and reducing repeatable triggers.
Progressive loading: build frequency first, then duration, then intensity.
Break up sitting: stand and move every 30 to 45 minutes.
Prioritise strength and control (not just flexibility): glutes, trunk endurance, and hip control often matter.
Sleep and stress: they can amplify pain, improving them can reduce flare frequency.
Frequently Asked Questions
What is the most common cause of lower back pain? Most lower back pain is “non-specific”, often linked to temporary tissue irritation, muscle guarding, and load exceeding your current capacity (for example, lifting, sitting, or sudden activity increases).
Is walking good for lower back pain? For many people with non-specific lower back pain, gentle walking helps reduce stiffness and supports recovery. Start small and increase gradually.
Heat or ice for lower back pain, which is better? Many people prefer heat for stiffness and muscle spasm, while some prefer ice shortly after a sudden strain. Use whichever helps you move more comfortably.
How long does acute lower back pain usually last? Many episodes improve within a few weeks. If pain is not improving, keeps recurring, or limits daily life beyond a couple of weeks, an assessment can help.
What sleeping position is best for lower back pain? Common comfort positions include side-lying with a pillow between the knees, or lying on your back with a pillow under the knees.
Get help for lower back pain in Central London
If your lower back pain is stopping you from working, training, or sleeping, an expert assessment can speed up recovery and reduce recurrences.
Versano Clinics in Central London offers personalised osteopathic care for pain relief and rehabilitation, with in-person and virtual consultations and same-day appointments when available.
Explore your options or book an appointment at Versano Clinics.

