Chronic Ache: When to Get Osteopathic Help in London
A persistent chronic ache can be easy to dismiss at first, especially in a busy city where long commutes, desk-based work, and high stress can make discomfort f...
Jan 29, 2026

A persistent chronic ache can be easy to dismiss at first, especially in a busy city where long commutes, desk-based work, and high stress can make discomfort feel “normal”. But when that nagging back, neck, shoulder, or hip ache starts shaping how you sleep, work, train, or even relax, it is worth taking seriously.
In clinic, the key question is rarely “Is this pain real?” It is “What is driving it, and what do we do next?” This guide explains when osteopathic help can be the right next step in London, what to watch for (including medical red flags), and what to expect from an osteopathic assessment.
What counts as a chronic ache?
People use “ache” for many sensations: stiffness, tightness, heaviness, soreness, or a dull throb. Clinically, pain is often described as chronic when it lasts 3 months or more, even if it varies day to day. The NHS uses this timeframe when discussing chronic pain and long-term symptoms.
There are two useful patterns:
Ongoing ache after an obvious trigger, such as lifting something heavy, a sports injury, or a period of intense stress.
A recurring ache with no single cause, often linked to posture, repetitive strain, or gradual deconditioning.
Either way, persistent symptoms can become a cycle: discomfort changes how you move, reduced movement increases stiffness and sensitivity, and the body becomes less tolerant of everyday loads.
When to move from self-management to professional help
Short-lived aches often respond to simple steps (appropriate movement, pacing, sleep, hydration, and sensible training modifications). What tends to predict the need for professional input is not just pain intensity, but duration, recurrence, and impact.
Consider booking an osteopathic assessment if your chronic ache:
Lasts longer than 2 to 6 weeks despite basic self-care, or keeps returning.
Affects sleep, concentration, mood, or confidence in movement.
Limits daily function, for example walking pace, driving, desk work, gym training, or childcare.
Is linked to posture or work habits, such as prolonged sitting, laptop use, or a repetitive job.
Flares with specific activities (running, lifting, cycling) and you want a clear plan to return safely.
Feels “stuck”, where stretching, rest, or occasional massage only gives short relief.
If you are trying to stay active, it can help to learn how to adjust load rather than stop completely. (Versano also covers practical movement habits in Why Staying Active Is Essential for Your Health.)
Important: when chronic ache should be checked urgently
Osteopaths are trained to screen for signs that suggest you should see a GP urgently, attend urgent care, or call emergency services. Do not “wait it out” if any of the following apply.
New bowel or bladder changes, numbness around the genitals or anus, or sudden severe leg weakness (possible cauda equina symptoms).
Chest pain, breathlessness, or pain spreading to the jaw/arm, or any symptoms suggesting a heart problem.
Unexplained weight loss, fever, night sweats, or feeling systemically unwell alongside your pain.
Significant trauma, especially in older adults, or possible fracture.
History of cancer, immunosuppression, or infection risk, with new severe pain.
Progressive neurological symptoms, such as worsening numbness, pins and needles, or weakness.
If you are unsure, start with your GP or NHS 111. For general guidance on back pain and when to seek help, the NHS is a reliable reference point.
When osteopathy is a good fit for chronic ache
Osteopathy commonly helps when the ache is primarily musculoskeletal, meaning related to joints, muscles, nerves, connective tissue, and movement patterns. Many people seek osteopathic care for back and neck pain, postural strain, headaches linked to neck tension, and sports or gym-related issues.
Osteopathic treatment is not about “chasing pain”. It is about identifying contributors (movement restrictions, load tolerance, strength and control, breathing patterns, stress, recovery, and ergonomics) and building a plan you can follow.
Here is a practical guide to deciding your next step.
What you notice | What it may suggest | A sensible next step |
|---|---|---|
Dull ache and stiffness that builds through the workday | Postural or repetitive strain, reduced movement variety | Osteopathic assessment and a plan for movement breaks, mobility and strength |
Pain that returns when you restart the gym or running | Load management issue, technique, mobility or control deficits | Osteopathy plus progressive rehab (often alongside physiotherapy principles) |
Persistent neck/upper back tightness with headaches | Cervicogenic contributors, stress and desk setup factors | Postural assessment, manual therapy, and targeted exercise |
Back pain with leg symptoms that are mild and stable | Possible nerve irritation that needs monitoring | Assessment to guide rehab and red-flag screening, refer if needed |
Pain that is worsening, constant, or associated with systemic symptoms | Non-musculoskeletal causes need ruling out | GP or urgent care first |
How osteopathy can help with chronic ache (what the evidence-based approach looks like)
Modern osteopathic care typically combines hands-on treatment with education and exercise-based rehabilitation.
1) A whole-person assessment, not just “where it hurts”
Chronic ache often involves multiple drivers: local tissue sensitivity, movement habits, stress, sleep quality, previous injury, and workload. A thorough assessment usually includes:
A detailed history (when it started, patterns, triggers, and what eases it)
Screening for red flags and referral needs
Physical tests for mobility, strength, control, and relevant neurological signs
2) Manual therapy to reduce sensitivity and improve movement options
Hands-on techniques (mobilisation, soft tissue work, and other manual approaches) can help calm symptoms for some people, particularly when combined with active rehab.
For low back pain, UK guidelines such as NICE recommend manual therapy only as part of a package including exercise, rather than as a stand-alone solution. That combination is often what helps symptoms stay improved between appointments.
3) Rehab that rebuilds tolerance, not just flexibility
Many chronic aches persist because the body has become less tolerant to a particular load, for example sitting, running, overhead work, or heavy lifting. Your plan may include:
Graded strengthening for key areas (hips, trunk, upper back, shoulders)
Mobility and control drills that match your goals
Pacing strategies to prevent boom-and-bust flare patterns
4) Postural assessment that focuses on habits and environment
In London, a large share of persistent neck and back ache is linked to long desk hours and commuting. A useful postural approach is practical, such as screen height, chair setup, bag choice, and how often you change position, rather than trying to “hold perfect posture” all day.
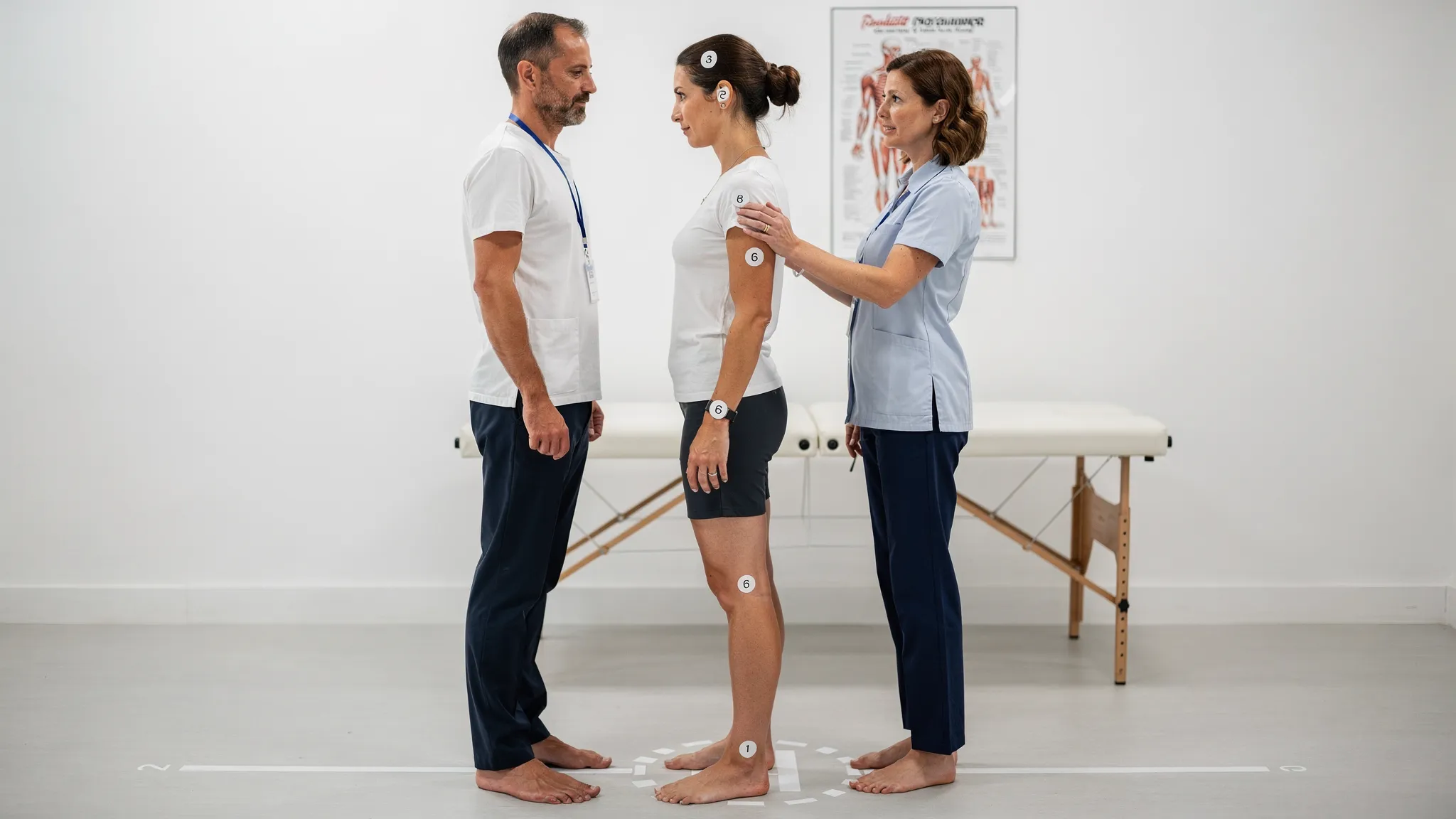
What to expect at an osteopathic appointment (and how virtual consults can work)
If you have never seen an osteopath before, the process should feel structured and collaborative. At Versano Clinics, treatment options include in-person care and virtual consultations, which can be especially helpful for busy schedules, flare-ups, or getting early guidance.
Part of the appointment | What typically happens | Why it matters for chronic ache |
|---|---|---|
Case history | Symptoms, patterns, medical background, goals | Helps identify drivers, rule out concerns, and personalise your plan |
Physical assessment | Movement tests, palpation, strength and control checks | Clarifies what is contributing to symptoms and what to target |
Explanation | Clear working diagnosis and what it means | Reduces uncertainty and improves adherence to the plan |
Treatment plan | Manual therapy (if appropriate), rehab exercises, pacing advice | Aims for durable change, not short-lived relief |
Follow-up strategy | What improvement should look like, when to review, when to refer | Keeps care safe, measurable, and goal-driven |
Virtual consultations can work well for: understanding symptoms, load management, exercise planning, desk and training modifications, and deciding whether an in-person exam is needed. Hands-on assessment and manual treatment, however, require an in-person visit.
Why early help can prevent a “small ache” becoming a long-term problem
Many people wait until the ache is severe. The problem is that chronic symptoms can become more complex over time, particularly if movement becomes guarded, sleep deteriorates, and stress rises.
Getting help earlier does not mean you are committing to lots of appointments. It often means you get:
A clearer explanation of what is happening
Guidance on what to stop doing (and what to keep doing)
A realistic timeline for recovery
A rehab plan that matches your life, work, and training
How to choose an osteopath in London (quick safety and quality checks)
In the UK, osteopaths are regulated. You can verify registration via the General Osteopathic Council (GOsC), which maintains the official register.
Beyond credentials, choose a clinic that:
Explains your condition and options in plain language
Screens for medical red flags and refers appropriately
Builds a plan around your goals, not a generic protocol
Can support rehab and progression (not only passive treatment)
Offers practical access (for example, same-day appointments when you are flaring)
If you want coordinated care, it can also help when a clinic offers related services such as physiotherapy, massage, and structured rehabilitation, so your plan stays consistent.

Frequently Asked Questions
How long should I wait before seeing an osteopath for a chronic ache? If an ache lasts more than 2 to 6 weeks, keeps recurring, or starts limiting sleep and function, an assessment is reasonable. If it has lasted 3 months or more, it is typically considered chronic and worth addressing with a structured plan.
Can osteopathy help if scans show “wear and tear” or disc changes? Often, yes. Imaging findings do not always match pain levels, and many people improve with a plan focused on movement, strength, and load management. An osteopath can explain what your results mean and guide safe progression.
Do I need a GP referral to see an osteopath in London? Usually no, you can self-refer. If your symptoms suggest a medical issue, your osteopath should advise seeing a GP or urgent care.
Is osteopathy suitable for sports injuries and gym-related pain? It can be, particularly when treatment is paired with a progressive rehabilitation plan. This is commonly used for overuse issues, return-to-training support, and movement-related aches.
What is the difference between osteopathy and physiotherapy for chronic ache? There is overlap. Both professions assess movement and support rehabilitation. Osteopathy often includes hands-on assessment and manual therapy alongside exercise and lifestyle advice. The best choice is the practitioner who offers a clear diagnosis, safety screening, and a plan you can follow.
Can I start with a virtual consultation? Yes, a virtual appointment can be a good first step for triage, advice, and exercise planning. If hands-on assessment is needed, you can then book in-person care.
Book osteopathic help for chronic ache in London
If you are dealing with a chronic ache that is limiting your work, training, or sleep, getting a clear assessment can be the turning point. Versano Clinics offers personalised osteopathic care in Central London, with same-day appointments (where available) plus virtual and in-person consultations, and support across osteopathy, physiotherapy, massage, and rehabilitation.
Explore options or request an appointment via Versano Clinics.

