MSK Issues Explained: Signs, Causes and Treatment Options
Musculoskeletal (MSK) issues are one of the most common reasons people seek help for pain, reduced mobility, or recurring “niggles” that won’t settle. They can ...
Jan 29, 2026

Musculoskeletal (MSK) issues are one of the most common reasons people seek help for pain, reduced mobility, or recurring “niggles” that won’t settle. They can affect your back, neck, shoulders, hips, knees, ankles, muscles, joints, tendons, ligaments and nerves, and they often show up at the worst possible time: during a busy work period, marathon training, or when you simply need to get on with daily life.
This guide explains what MSK issues are, the most common signs and causes, and the treatment options that tend to work best (from self-management and rehab to osteopathy and physiotherapy). It also covers when symptoms should be checked urgently.
What are MSK issues?
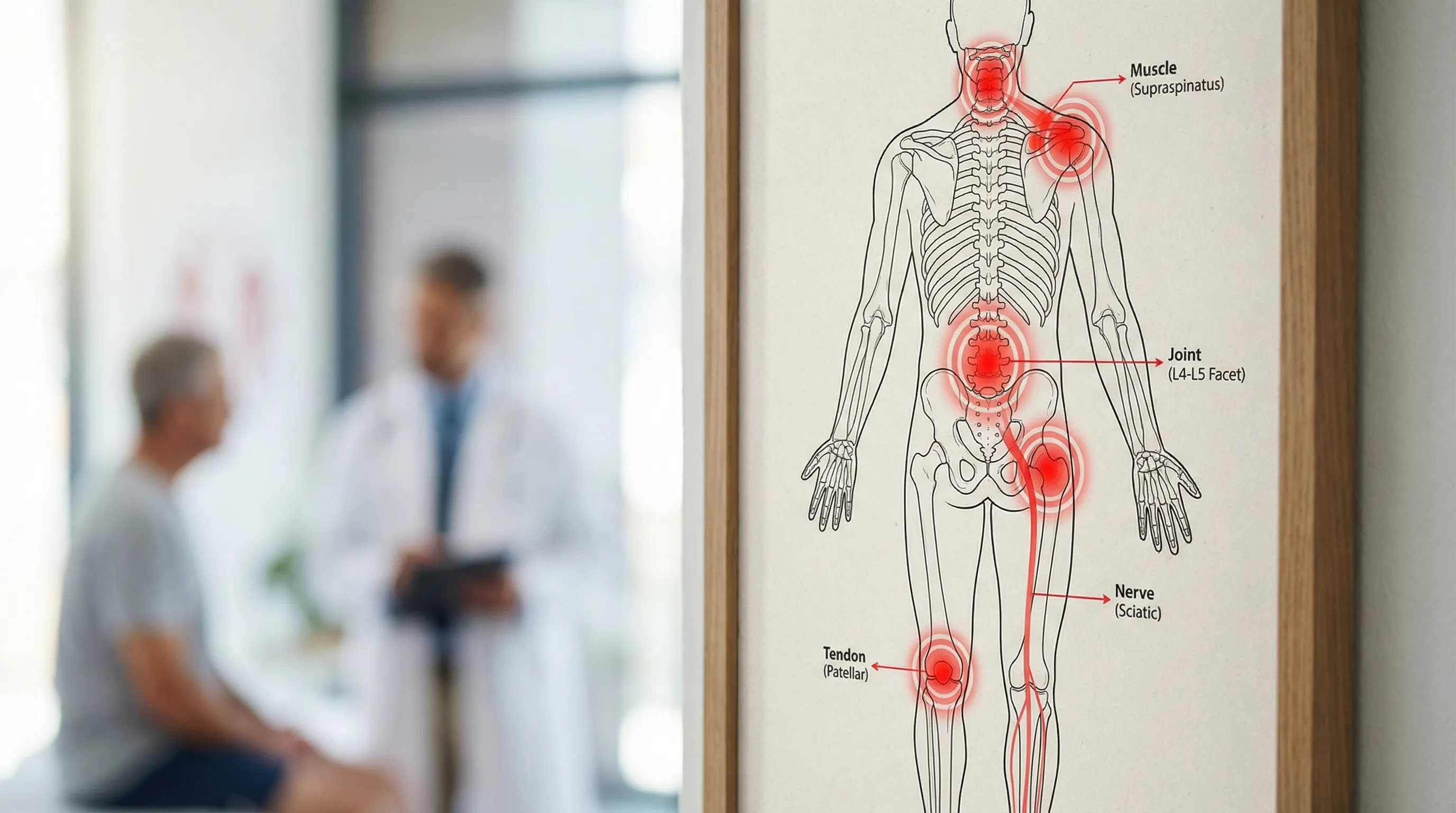
“MSK” is short for musculoskeletal. MSK issues describe problems involving:
Muscles (strains, tightness, trigger points)
Joints (irritation, stiffness, osteoarthritis)
Tendons and ligaments (tendinopathy, sprains)
Bones (stress reactions, fractures)
Nerves (irritation, compression, referred pain)
MSK pain is not always caused by a single “injury”. Many cases develop gradually due to a combination of load, posture, stress, sleep, previous injury, and general conditioning. The good news is that most MSK problems respond well to a structured plan.
Signs and symptoms of MSK issues
MSK symptoms vary depending on the tissue involved and where the problem sits (for example, neck pain can refer into the shoulder or arm). Common symptoms include:
Pain (sharp, dull, aching, burning, or throbbing)
Stiffness, especially after rest or first thing in the morning
Reduced range of movement (turning your head, reaching overhead, bending)
Weakness or a feeling of instability
Swelling, warmth, or tenderness around a joint or tendon
Pins and needles or numbness (often suggests nerve involvement)
Symptoms that flare with specific activities (running, desk work, lifting)
MSK pain or something more serious? (Red flags)
Most MSK pain is not dangerous, but certain symptoms should be assessed urgently. The NHS provides clear guidance on when to seek urgent help for back pain and neurological symptoms.
Symptom | Often linked to | Get medical advice urgently if… |
|---|---|---|
New back or neck pain after a fall/trauma | Sprain/strain, fracture (less common) | Severe pain, visible deformity, or you are at risk of fracture (for example, osteoporosis) |
Pain plus fever, unexplained weight loss, or feeling very unwell | Infection/inflammation (needs checking) | Symptoms are significant or worsening |
Pain going down the arm/leg | Referred pain or nerve irritation | Progressive weakness, worsening numbness, or loss of coordination |
Bowel or bladder changes with severe back pain | Possible cauda equina syndrome | Any loss of bladder/bowel control, numbness in the saddle area, or severe worsening leg weakness |
Chest pain with arm/shoulder pain | Non-MSK causes possible | Any chest pressure, breathlessness, sweating, nausea |
If you have red flag symptoms, seek urgent medical advice (NHS 111 or A&E depending on severity). For back pain red flags, see the NHS guidance on back pain.
What causes MSK issues?
MSK issues usually come from one or more of these drivers:
1) Overload and under-recovery
A classic pattern is doing “too much too soon”, such as increasing training volume, starting a new gym programme, moving house, or returning to sport after time off. Tissue adapts, but it needs appropriate progression and recovery.
2) Repetitive strain and sustained postures
Long hours at a desk, driving, or manual work can irritate joints and soft tissues, particularly in the neck, shoulders, upper back, and lower back.
3) Previous injury and compensation
After an ankle sprain, for example, altered movement patterns can persist and shift load to the knee, hip, or back. This can show up months later as a “new” problem.
4) Age-related changes (plus what matters most)
Normal age-related changes in joints and discs are common and do not always correlate with pain. What often matters more is strength, movement variability, sleep quality, stress load, and graded activity.
5) Inflammation and systemic contributors
Some MSK symptoms are influenced by inflammatory conditions, metabolic health, or wider medical issues. If pain is widespread, persistent, and associated with fatigue or other systemic symptoms, it is worth discussing with a GP.
Common MSK problems (and how they typically feel)
These are among the most frequent MSK presentations in clinic:
Back pain
Back pain can be mechanical (movement related), disc-related, joint related, or driven by muscle and load tolerance. The majority of acute episodes improve, but recurrence is common without a plan.
Neck pain and headaches
Neck stiffness, pain with turning, and symptoms aggravated by screens or stress are common. Some headaches can be cervicogenic (originating from the neck), though headaches should be assessed carefully if patterns change.
Shoulder pain
Shoulder symptoms often involve the rotator cuff, biceps tendon, or the way the shoulder blade moves. Pain with reaching overhead, dressing, or sleeping on one side is a frequent complaint.
Hip, knee, and ankle pain
Running-related issues, tendinopathies, ligament sprains, and joint irritation are common. Load management and progressive strengthening are usually central to recovery.
Tendinopathy (for example, Achilles, patellar, tennis elbow)
Tendinopathy is often a “too much, too soon” or “too little, then suddenly too much” scenario. It usually responds best to progressive loading rather than complete rest.
Nerve-related symptoms (sciatica-like pain)
Pain that travels, plus tingling or numbness, can suggest nerve irritation. A proper assessment helps clarify whether the nerve is sensitised, compressed, or simply reacting to local tissue irritation.
How MSK issues are assessed
A good MSK assessment aims to answer three questions:
What structure(s) are most likely involved?
What is driving the problem now (load, movement, recovery, stress, ergonomics)?
What plan will restore function and reduce recurrence risk?
Assessment commonly includes:
Detailed history (onset, aggravating factors, previous injuries, training/workload)
Movement testing and range of motion
Strength and control testing
Neurological screening if there are nerve symptoms
Postural and functional assessment (particularly relevant for desk-based pain)
Imaging is not automatically required for MSK pain. Many guidelines recommend imaging only when it changes management, particularly where red flags exist or symptoms are not improving as expected. For example, NICE guidance for low back pain and sciatica emphasises exercise and a structured approach rather than early imaging for most people. See NICE guideline NG59.
Virtual consultations can be useful for triage, movement assessment, exercise progressions, and ergonomic set-up, especially when in-person care is not immediately convenient.
Treatment options for MSK issues
The best treatment usually combines short-term symptom relief with longer-term capacity building (strength, mobility, confidence, and load tolerance).
Self-management (often the foundation)
Depending on your presentation, self-management may include:
Relative rest (reducing the provoking activity rather than stopping all movement)
Gradual return to normal activity, as tolerated
Heat or cold for symptom relief
Improving sleep routine and recovery habits
Simple mobility and strengthening work
If you are unsure what is safe to do, professional guidance helps you stay active without repeatedly flaring symptoms.
Exercise-based rehabilitation
For many MSK issues, progressive exercise is one of the most evidence-supported approaches. Rehab targets:
Strength (often under-loaded muscles around the painful area)
Mobility (when stiffness is relevant)
Control and coordination (especially after injury)
Sport-specific or work-specific tolerance (graded exposure)
Manual therapy (including osteopathy)
Manual therapy can be helpful for pain modulation, movement confidence, and short-term symptom relief when integrated into a broader plan.
Osteopathic treatment may include hands-on techniques for joints and soft tissues, alongside advice and exercises. Some people also explore approaches such as cranial or visceral osteopathy depending on presentation and clinician reasoning.
Physiotherapy
Physiotherapy is particularly valuable for structured rehab, return-to-sport planning, and progressive strengthening after acute injury or persistent pain.
Massage (sports and deep tissue)
Massage can reduce perceived muscle tension and soreness, and can complement rehab when used strategically (for example, when pain is limiting movement). It is usually most effective when it supports, rather than replaces, a progressive strengthening plan.
Medication and injections (when appropriate)
Some people benefit from short-term pain relief to enable movement and sleep. Medication choices should be discussed with a pharmacist or GP, especially if symptoms are persistent, severe, or you have other health conditions.
In selected cases, injections (such as corticosteroid injections) may be considered by appropriate clinicians, typically when conservative care is not enough and the diagnosis supports it.
Surgery (rare, but sometimes necessary)
Surgery is usually reserved for specific diagnoses, significant structural problems, or progressive neurological deficits. Most MSK issues are managed conservatively first.
Treatment options at a glance
Treatment option | Best suited to | What to expect |
|---|---|---|
Education and load management | Most MSK pain, especially recurring flare-ups | A plan to reduce irritation while staying active and rebuilding tolerance |
Rehab exercises | Tendinopathy, back/neck pain, post-injury rehab | Progressive strengthening and functional goals (work, sport, daily tasks) |
Osteopathy (hands-on + plan) | Back/neck pain, movement restriction, multi-factor pain | Symptom relief plus guidance on movement, posture, and progression |
Physiotherapy | Sports injuries, return to sport, post-operative care | Structured rehab, reconditioning, and measurable milestones |
Sports/deep tissue massage | Muscle-dominant discomfort, training soreness | Short-term relief to support movement and recovery |
Medications (via GP/pharmacist advice) | Acute pain affecting sleep/function | Short-term symptom control to keep you moving |
When should you seek help for MSK issues?
Consider a professional assessment if:
Pain persists beyond 1 to 2 weeks with little improvement
You keep getting the same flare-up (for example, back pain every few months)
Symptoms limit work, training, or sleep
You have pins and needles, numbness, or weakness
You are unsure what movements are safe (and fear is keeping you inactive)
Early support is not just about “fixing pain”. It is about identifying the drivers and reducing the chance that a small issue becomes a long-term limitation.
Preventing MSK issues (and reducing recurrence)
Prevention is rarely about perfect posture or avoiding all strain. It is about improving capacity and recovery so your body tolerates the life you actually live.
Helpful strategies include:
Build general strength (especially legs, hips, and upper back) alongside mobility
Increase training gradually, and avoid sudden spikes in volume or intensity
Break up long sitting with micro-movement (short walks, gentle mobility)
Prioritise sleep and recovery, particularly during high stress periods
Maintain regular physical activity you can sustain year-round
If you want practical ideas for staying consistent, see Versano’s guide on why staying active is essential for your health.

Frequently Asked Questions
What does MSK stand for? MSK stands for musculoskeletal and refers to issues affecting muscles, joints, tendons, ligaments, bones, and sometimes nerves.
How do I know if my pain is muscular or nerve-related? Muscular pain is often local and sore with pressure or movement. Nerve-related symptoms more often include tingling, numbness, burning pain, or pain that travels into an arm or leg. A clinical assessment can help clarify the driver.
Do MSK issues always need imaging (MRI or X-ray)? No. Many MSK conditions are diagnosed clinically, and imaging is usually reserved for red flags, suspected fracture, significant neurological signs, or when results will change management. NICE guidance for low back pain supports a conservative approach for most people.
Is osteopathy good for MSK issues? Osteopathy can be helpful for MSK issues, particularly when hands-on treatment is combined with advice, exercise, and a personalised plan to address contributing factors.
Should I rest completely if I have MSK pain? Complete rest is rarely the best approach. Relative rest and graded activity are typically more effective, unless a clinician advises otherwise (for example, after a fracture or certain acute injuries).
Book an MSK assessment at Versano Clinics
If you are dealing with persistent pain, a recurring injury, or stiffness that keeps returning, a structured plan can make a big difference. Versano Clinics is a modern osteopathic clinic in Central London offering personalised MSK care including osteopathy, physiotherapy, postural assessment, rehabilitation programmes, and sports/deep tissue massage. Same-day appointments and virtual consultations are available, and major insurance is accepted.
Learn more or book via the Versano Clinics website.

